
The success of our Brain in Hand trial at Cedar House prompted us to consider how else we can use this piece of technology.
Next stage of development for Brain in Hand at Cedar House
Brain in Hand (www.braininhand.co.uk) is currently being used to help patients better self-manage in order to reduce anxiety and crisis incidents, especially when in the local community.
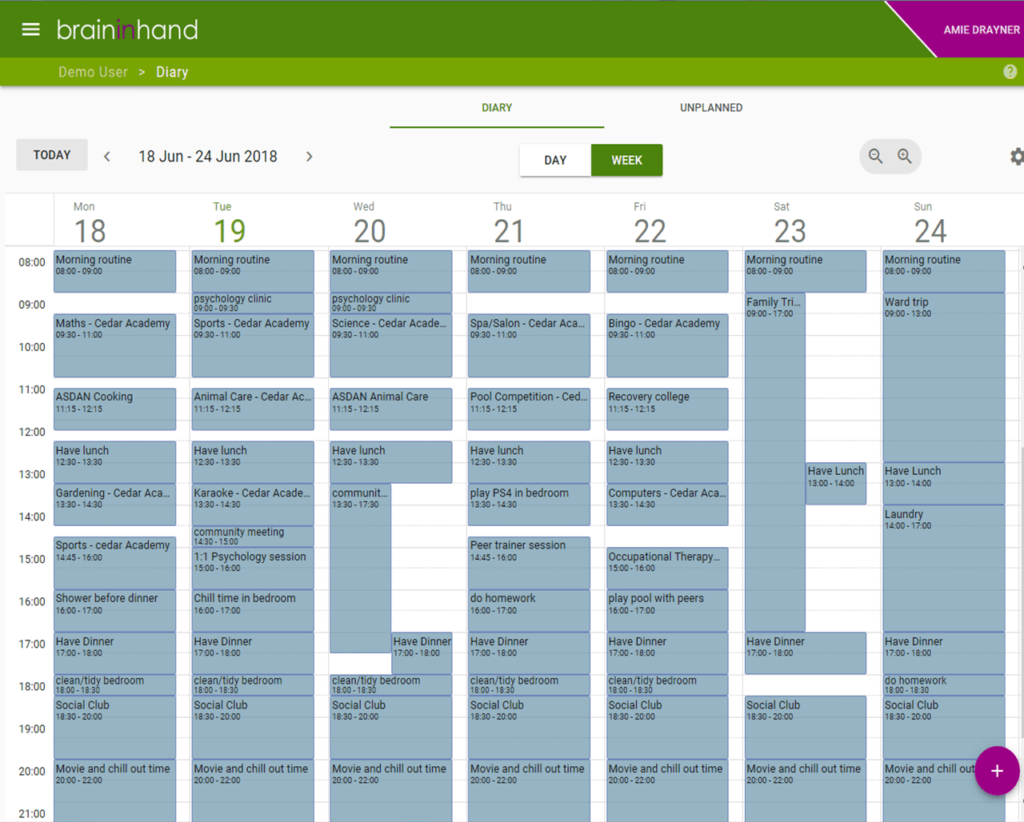
Brain in Hand gives patients easy access to their own personalised diary, reminders, and coping strategies through an app on their phone. An inbuilt anxiety monitor also allows users to report their emotional state on a regular basis using a simple traffic light system. This enables support staff to be able to see how patients are feeling, wherever they are, and intervene if needed.
If coping strategies aren’t working and a patient needs help, they can press the red traffic light button at any time and a text message is sent to the allocated phone holder. The allocated phone holder then contacts a trained traffic light responder, who will get in touch with the patient to help to de-escalate the problem. The system also provides a wealth of usage data, including anxiety tracking and problems faced, to help with reflection and planning.

And now we’re developing the app so that staff can use it for patients who are unable to use it themselves. The app is set up so that every single item in a patient’s diary is logged, with each individual step of every item logged. This facilitates absolute continuity of care with incidents minimised or potential ‘crisis points’ managed in the best way possible.
Whilst the idea of an itemised diary may seem fairly straightforward, for some of our patients, particularly those with autism, it is far from that. Some of our patients require an extremely structured approach, with the exact same steps and words to their routine every day. Every question must receive the ‘correct’ answer, phrased using the ‘correct’ words or confusion, frustration and high levels of anxiety for both staff members and patients can ensue.
The Brain in Hand app ensures that all team members understand every step of the patient’s day in finite detail and will know what trigger points may exist and how best to manage them.
But the app does more than that. It enables team members to track responses to suggested solutions using a traffic light system. Tracking of responses is then reviewed and suggestions for solutions refined based on what has been proven to work best. Again, this detailed history of what works and when ensures much greater consistency of care, which is critical for some of our more challenging patients.
The end result is settled patients, fewer incidents and hugely reduced pressure on team members. Detailed Diaries (which can take days or even weeks to enter fully) are currently being created for a small number of patients. The team hope to be able to start using the app fully from the end of September. This realistic time scale will enable the team enough time to think of as many potential problems/behaviours and solutions as possible, so that once the app is launched, it is as reliable as possible.
